
5 Things You Didn’t Know About Oral Health Disparities in Latin America
In a hillside community outside Quito, a mother walks more than an hour to reach a temporary outreach clinic. Her son has been complaining about tooth pain for months. The nearest permanent dental facility is difficult to access, and missing work for travel means losing income.
Stories like this illustrate how oral health disparities are not only about cavities or cleanings. They are about infrastructure, income, prevention, and access to consistent care.
Understanding oral health disparities in Latin America requires looking beyond individual behavior and examining the broader systems that shape health outcomes.

1. Oral Health Disparities Reflect Larger System Gaps
A simple health disparity definition describes differences in health outcomes between populations linked to social, economic, or environmental disadvantage. In practice, these differences are deeply interconnected.
Limited access to clean water, transportation barriers, food insecurity, and gaps in public infrastructure all affect oral health. In many low-income communities, families prioritize urgent needs such as housing or employment over preventative dental visits.
This is why oral health disparities often mirror broader inequalities within healthcare in Latin America. Rural and peri-urban communities may have fewer providers, longer travel times to clinics, and limited preventative programming.
To understand why oral health is inseparable from public systems, explore why oral health is a public health issue.

2. Prevention Is Often Less Accessible Than Emergency Care
Many public systems in Latin America provide emergency dental treatment, but consistent preventative care can be harder to access. Screenings, fluoride treatments, and oral health education are essential to reducing long-term disease, yet they are not always evenly distributed.
When prevention is inconsistent, small issues become advanced problems. Children may miss school due to untreated pain. Adults may delay care until infections interfere with work.
Organizations focused on long-term development emphasize prevention as the first step in reducing oral health disparities. Screenings and education connect patients to follow-up care rather than offering isolated procedures.
You can read more about how access to dental care impacts children’s education and development.

3. Geography Plays a Major Role in Healthcare in Latin America
Healthcare in Latin America varies widely between urban centers and rural communities. While major cities may have specialty clinics and dental schools, remote areas often face provider shortages.
In hillside or rural regions, infrastructure can directly affect access. Lack of safe roads or staircases makes routine visits physically difficult. In some partner communities, development projects such as staircases or retention walls have improved safe access to clinics, indirectly reducing oral health disparities by making care reachable.
These examples show that oral health is shaped by the built environment as much as by clinical expertise.
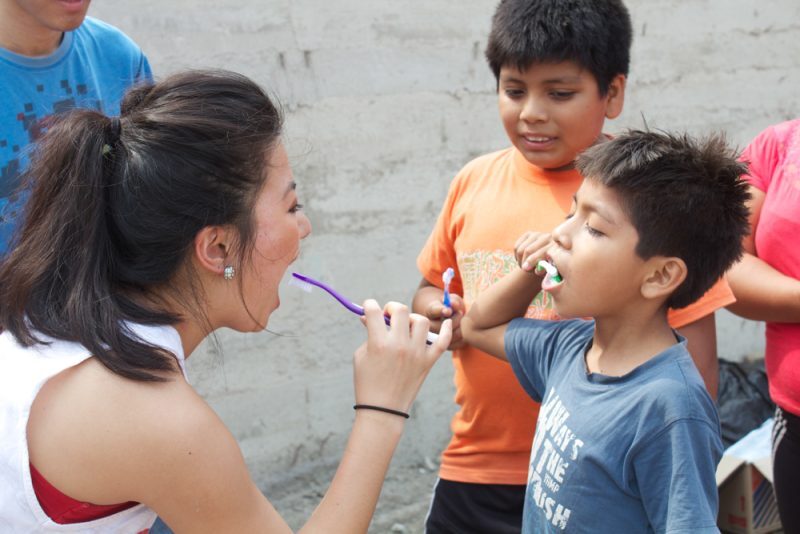
4. Education and Cultural Context Matter
Oral health education must be culturally responsive and community-driven. Messaging that works in one setting may not translate directly to another.
Local providers understand language, traditions, and barriers that influence daily habits. Community-led workshops often focus on practical prevention strategies that families can realistically maintain.
Ethical engagement means supporting licensed local professionals and reinforcing existing public systems. If you are exploring service opportunities, learning about ethical standards in dental volunteer programs can help you evaluate program quality.

5. Long-Term Partnerships Reduce Oral Health Disparities More Effectively Than Short-Term Missions
Short-term missions may provide temporary relief, but sustained partnerships are more likely to reduce oral health disparities over time.
Through long-term collaboration with local leaders, year-round staff, and public health systems, organizations can:
- Conduct consistent screenings
- Provide preventative education
- Refer patients for follow-up treatment
- Invest in infrastructure that improves access
This approach aligns with Sustainable Development and Community Empowerment principles. Rather than replacing local systems, it strengthens them.
Students who participate in structured service learning trips often gain a deeper understanding of how oral health disparities connect to housing, education, and economic opportunity. You can read reflections on how volunteer experiences build clinical confidence while reinforcing ethical practice.
Why Understanding Oral Health Disparities Matters for Future Healthcare Leaders
For students interested in Global Health, recognizing the root causes of oral health disparities is essential. Addressing inequity requires more than clinical skill. It requires collaboration, prevention, and long-term thinking.
Reducing oral health disparities takes patience, partnership, and persistence. With thoughtful engagement, students and supporters can contribute to long-term systems that improve health outcomes across communities.
Join the Smiles Movement to Promote Oral Health
If you are interested in learning more about structured service learning experiences, consider downloading the Smiles Movement brochure to explore upcoming opportunities.
If you would like to support sustainable, community-driven programs that address oral health disparities at their root, you can support MEDLIFE’s Moving Mountains initiative. Ongoing contributions help maintain preventative clinics, infrastructure improvements, and partnerships that expand access to care.




